Introduction
Hunter Syndrome is a rare genetic disorder that affects mostly young boys in the United Kingdom. Though it is uncommon, awareness about hunter syndrome in UK is growing among UK families and medical professionals. People often confuse it with hantavirus disease or other conditions, but they are completely different. Hunter Syndrome is also known as hunter syndrome mps type 2, and it belongs to a group of conditions called mucopolysaccharidoses (MPS).
In this detailed UK-focused guide, we explain the hunter syndrome cause, symptoms, hunter syndrome clinical features, diagnosis, treatment options, hunter syndrome inheritance, and the current situation in the UK. The aim is to share knowledge in a friendly way and help families find hope, guidance, and support from hunter syndrome support groups in the UK.
Let’s understand this condition step by step.
What Is Hunter Syndrome? – Meaning in Simple Words
Hunter syndrome meaning: It is a rare genetic disorder where the body cannot break down certain sugars called mucopolysaccharides due to the lack of a specific enzyme. This causes physical and neurological symptoms. The scientific name is MPS II, and the hunter’s syndrome life expectancy depends on how early treatment begins.
Since enzyme deficiency is the main issue, many UK specialists offer hunter syndrome enzyme replacement therapy to manage symptoms. However, there is no permanent cure yet. It differs from hunter’s disease from mice, which refers to hantavirus disease, a separate infection caused by rodent exposure. These two must not be confused.
Hunter Syndrome Incidence in the UK
Studies show that hunter syndrome incidence is around 1 in 100,000 to 1 in 150,000 births in the UK. Medical research indicates that hunter syndrome infant symptoms often appear during the first 2-4 years of life. Because it is X-linked, hunter syndrome female cases are extremely rare, but females can be carriers.
Doctors often use bow hunter’s syndrome icd 10 code G45.0, for differential diagnosis, especially when symptoms relate to blood flow issues in the brain or neck. However, bow hunter’s syndrome is different and mostly neurological, while hunter syndrome MPS type 2 is metabolic and genetic.
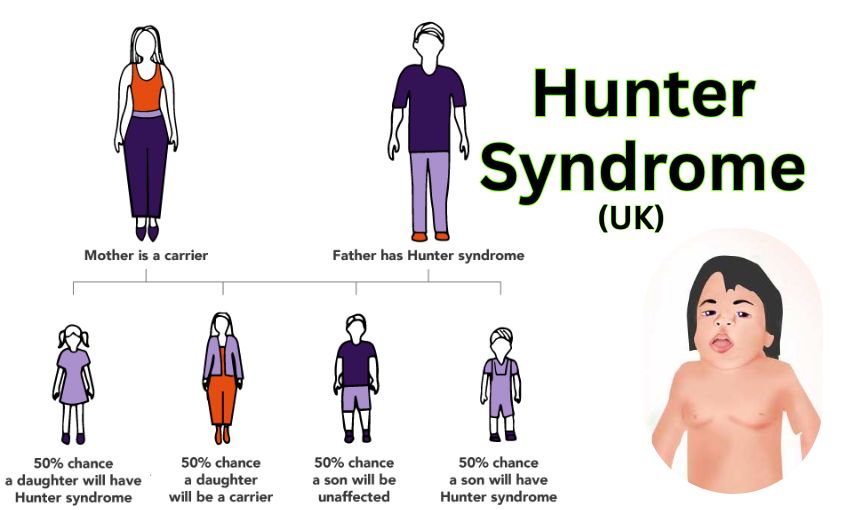
Hunter Syndrome Mode of Inheritance
The hunter syndrome mode of inheritance is X-linked recessive, meaning boys are mostly affected while girls can be carriers. A single gene mutation leads to enzyme deficiency. This makes hunter syndrome cause genetic and not related to infection or lifestyle. Parents often ask if it comes from hunter syndrome the voice singer Sean Millis, as he raised awareness by speaking openly about his journey with the condition. His story inspired many UK families to seek information early.
Hunter Syndrome Clinical Features
Here are the most common hunter syndrome clinical features found in UK cases:
| Physical Features | Neurological Features | Other Concerns |
| Coarse facial features | Developmental delay | Hunter syndrome hearing loss |
| Hunter syndrome skin thickening | Behavioural issues | Breathing difficulty |
| Enlarged head or liver | Learning challenges | Joint stiffness |
| Pebbled skin (hunter syndrome pebbling) | Slowed speech | Vision problems (hunter syndrome eye findings) |
The condition progresses differently in every child. Some children show hunter syndrome mild symptoms, while others develop severe issues requiring full-time care.
Hunter Syndrome Symptoms – Early Warning Signs
Parents must look out for the following hunter syndrome symptoms:
- Thick skin and facial changes
- Frequent ear infections
- Enlarged tongue
- Delayed walking or talking
- Enlarged abdomen
- Joint stiffness
- Slow growth
- Thick eyebrow ridge
- Breathing problems
- Hunter syndrome hearing loss
The hunter syndrome differential diagnosis includes autism, muscular dystrophy, hunter’s disease symptoms, and metabolic disorders. Hence, early medical evaluation is essential.
Diagnosis of Hunter Syndrome in the UK
Diagnosis usually involves:
- Urine test – to detect mucopolysaccharides
- Blood enzyme test – checks for enzyme deficiency
- Genetic test – confirms hunter syndrome inheritance pattern
- MRI / CT scans – for neurological damage
- Ophthalmic test – to check hunter syndrome eye findings
The NHS offers genetic counselling for affected families. Private diagnostic labs in London, Manchester, and Birmingham also provide MPS II testing.
Hunter Syndrome Treatment Options in the UK
Though there is no complete cure, many hunter syndrome treatment methods help improve life quality.
1. Enzyme Replacement Therapy (ERT)
The most used method is hunter syndrome enzyme replacement. The medication Idursulfase helps break down waste material in cells. It is administered via IV infusion.
2. Physiotherapy and Occupational Therapy
These therapies help with mobility, communication, and sensory improvement.
3. Surgery (if needed)
Sometimes children need surgeries to correct heart issues, breathing problems, or hernias.
4. Specialist Clinics in the UK
Several hospitals offer Hunter Syndrome care:
- Great Ormond Street Hospital, London
- Royal Manchester Children’s Hospital
- Birmingham Children’s Hospital
- Evelina London Children’s Hospital
These hospitals are highly experienced in hunter disease symptoms management and rare genetic disorders.
Hunter Syndrome Dietary Changes
Although diet cannot cure the condition, hunter syndrome dietary changes can improve digestion, gut function, and immunity. UK diet specialists recommend:
High-fibre foods
Fresh fruits and vegetables
Omega-3 foods (flaxseed, salmon, walnuts)
Soft-texture foods for children with swallowing difficulty
Avoid processed sugar, fried foods, or chemical preservatives. A proper hunter syndrome diet plan supports overall health and improves metabolism.
Hunter Syndrome Support Groups in the UK
Families dealing with rarity often feel alone. Thankfully, many hunter syndrome support groups in the UK provide emotional guidance, financial help, and medical resources. Some leading support networks include:
- MPS Society UK
- Rare Disease UK
- Genetic Alliance UK
- Children’s Hospital Networks
- NHS Rare Disorders Helpline
These communities help families connect and share experiences about hunter’s syndrome and hunter syndrome life expectancy challenges.
Hunter Syndrome Lifespan & Prognosis
Hunter syndrome lifespan depends on symptom severity and treatment timing. Children with hunter syndrome mild symptoms may lead longer, semi-independent lives, while severe hunter’s disease symptoms may reduce mps ii life expectancy.
Average hunter disease life expectancy:
| Condition Severity | Average Life Span |
| Mild (managed) | 30–40+ years |
| Moderate | 15–20 years |
| Severe (untreated) | 10–15 years |
With good care, hunter’s syndrome life expectancy is improving in the UK. Advances in medicine and early diagnosis offer new hope to families.
Hunter Syndrome vs Hantavirus Disease – Not the Same!
Many people confuse hunter’s disease with hantavirus disease, or hunter’s disease from mice, but they are unrelated.
| Hunter Syndrome | Hantavirus Disease |
| Genetic disorder | Viral infection |
| No link to mice | Spread via mice droppings |
| Enzyme deficiency | Respiratory illness |
| Long-term care needed | Treated with antiviral therapy |
| hunter syndrome mps type 2 | hunter’s disease from mice |
Both are serious, but only one is inherited genetically — hunter syndrome mode of inheritance is X-linked, while hantavirus disease is caused by rodent exposure.
Hunter Syndrome & The Voice – Sean Millis Story
Hunter syndrome the voice gained attention when Sean Millis, a contestant on The Voice Australia, openly talked about his diagnosis. His resilience inspired millions worldwide. Though not from the UK, his story supports awareness of hunter syndrome clinical features and encourages people to stay positive.
Summary – Hunter Syndrome in the UK
Hunter Syndrome is rare but manageable with early diagnosis. UK researchers are working on gene therapy, while NHS teams provide ongoing support. Awareness campaigns and hunter syndrome support groups help families find strength, guidance, and compassion.
10 FAQs on Hunter Syndrome in the UK
1. What is hunter syndrome meaning in simple language?
It is a genetic disorder where the body cannot break certain sugars due to lack of an enzyme.
2. What is the hunter syndrome cause?
It is caused by a mutation in the IDS gene, passed through X-linked inheritance.
3. What is hunter syndrome incidence in the UK?
Approximately 1 in 100,000–150,000 births in the UK.
4. What are common hunter syndrome symptoms?
Thick skin, joint issues, slow growth, hearing problems, and facial changes.
5. Can a hunter syndrome female have this condition?
Very rare. Females are usually carriers because of the X-linked pattern.
6. Is hunter syndrome treatment possible in the UK?
Yes. Enzyme replacement therapy is used along with therapies and support care.
7. What are hunter syndrome eye findings?
Cloudy corneas, visual impairment, and retinal changes.
8. What is hunter’s syndrome life expectancy?
It depends on severity. Mild cases may reach 40+ years, while severe cases live shorter.
9. Are hunter syndrome dietary changes helpful?
Yes, they support digestion, immunity, and overall health.
10. Where can I find hunter syndrome support groups?
MPS Society UK, Rare Disease UK, NHS genetic support teams, and online communities.